Why Is My Pinky Toe Sideways? Causes and Treatment Options
Learn why your pinky toe turns sideways, common causes, and treatment options to relieve discomfort and prevent progression.

When people discover I am a Podiatrist they often bring up how “in demand” my profession is. They often base this on how many people they know with foot problems. Their sister the marathon runner, their neighbor with shin splints, their high school teenager with sports injuries. What most people do not realize is that a very high percentage of podiatry patients are diabetics! When people think of diabetic health issues they often think of heart, kidney or eye problems. However, the #1 reason for hospitalizations among diabetics are diabetic foot infections.
Diabetes effects the body’s ability to break down sugar. With excess sugar in the blood stream, the blood becomes “sticky”, like after a bottle of coke spills on the tile floor. The sticky blood then has a difficult time making it into the small blood vessels of the body-most commonly the eyes, heart, kidneys and FEET.
When the feet have decreased blood circulation to their small blood vessels, a myriad of problems occur.

1) Neuropathy: high sugar content in the blood “eats away” at the nerves of the feet, often resulting in painful numbness called neuropathy. The big problem here is that diabetic patients lose their protective sensation. Many patients walk around and step on sharp objects on their floors. I know of a patient who came to the hospital with third degree burns on the bottom of his feet because he took a cell phone call outside barefoot for 30 minutes in 100 degree heat. With neuropathy, patients do not even realize that a problem is there until it is too late. This situation leads to diabetic foot ulcerations.

2) Infection: with decreased blood flow to the foot the body has a more difficult time fighting infection. Your blood carries white blood cells which find, fight and destroy bacteria. Blood cells are also necessary in wound healing. Without healthy blood, ulcers can’t fight infection and can’t heal.
3) Gangrene: the scariest word ever, right? Gangrene simply put is dead tissue. Given the information above you can see how this all ends up here. Numbness leads to ulcers, ulcers get infected and can’t heal. When this gets far enough and no blood flow occurs, tissue dies and when tissue dies it often requires amputation. I have elected to leave out the statistics of diabetic limb amputations as they can be overwhelming. For more information on diabetic statistics click here

Each of these can occur independently, but the goal is to avoid them all. Controlling blood sugar through diet, having regular foot exams, evaluating blood flow and watching for signs of local infection (redness, warmth, drainage).
Podiatrists are on the forefront of taking care of the diabetic foot. It must be a team approach. Podiatrists collaborate with infectious disease, internal medicine and cardio-vascular surgery. Together as a team the diabetic foot can be healed and the ever dreaded amputations are avoided.
As always, never self diagnose and always consult with your doctor before starting any treatment. Also… lay off the sugar.
Foot and Ankle Specialists of The Woodlands offers comprehensive care for the diabetic foot. We specialize in diagnosing and treating all diabetic foot conditions whether it is medically or surgically. Dr. Marcin N. Vaclaw has experience in wound care, treating neuropathy diabetic foot pains and many other conditions. For more information on Diabetes and how it can affect the feet please contact us at
Foot and Ankle Specialists of The Woodlands
9191 Pinecroft Drive #150
The Woodlands, TX 77380
281.909.7722
info@FASthewoodlands.com
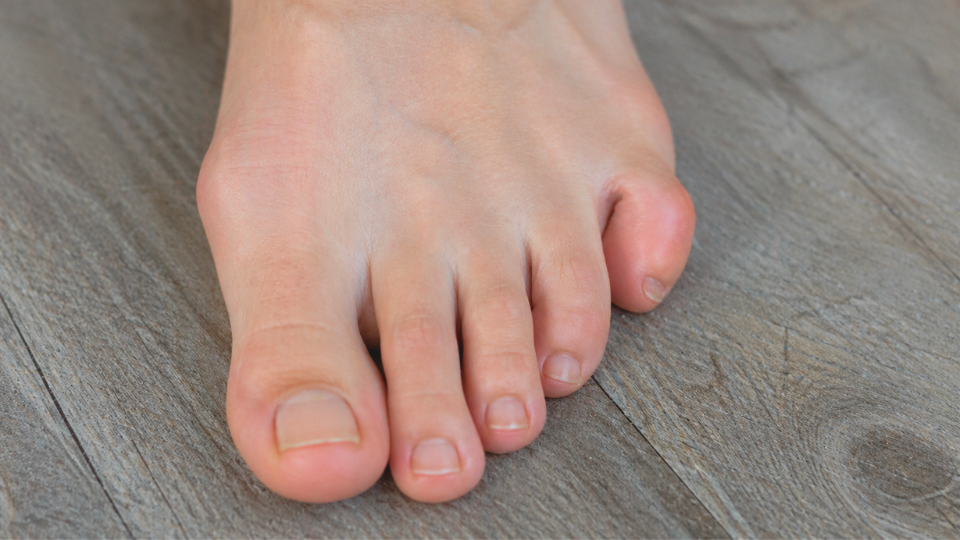
Learn why your pinky toe turns sideways, common causes, and treatment options to relieve discomfort and prevent progression.
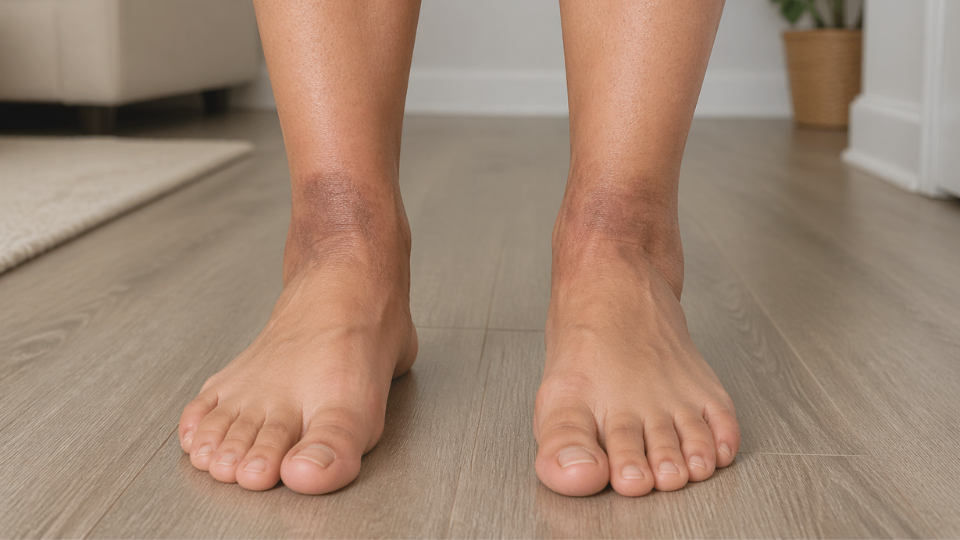
Learn what causes ankle discoloration, including dark spots and black ankles, and when to seek care for possible circulation issues.